Care workers and catering staff in residential care homes are facing challenges affecting their residents’ nutritional status. The way food is prepared, served and eaten in care homes has changed because of social distancing, pressures on carers and a lack of additional mealtime support from outside helpers e.g. visiting family.
Identifying malnutrition
Malnutrition is poor nutrition; described as a lack of energy, protein, and nutrient intake. Malnutrition affects every system in our body including the immune system, temperature regulation and other major organs.
It is recommended practice for all residents to be screened for malnutrition on admission into a residential care home, and monthly after that. The MUST tool is usually used to assess nutritional status but during these challenging times, this may not always be possible.
An alternative tool, the Patients Association Nutrition Checklist can be used to identify the potential risk of malnutrition.
Care homes should follow local guidance for managing residents at risk of malnutrition and put actions into place to address weight loss. This will often be in the form of a person-centred nutrition care plan.

Malnutrition and Covid-19
Malnutrition has been a concern in care homes during better times but is a bigger issue in the current pandemic climate.
Care home residents are likely to be eating and drinking less during the pandemic for the following reasons:
- Social isolation – residents now eat alone in their rooms
- Less support around mealtimes due to stretched staffing levels and risk management
- Supporting family members not currently visiting to help during mealtimes
- Distress, fear, and anxiety associated with developing symptoms of Covid-19
- Less will be known about new residents’ food likes and preferences
- Reduced menus and less access to a variety of foods
- Limited social interaction with other residents, carers, and family
Food for residents who are unwell with Covid-19
There is a definite increase of risk of malnutrition in people with Covid-19 due to:
- Poorer appetites
- Increase in energy required to fight the virus
- If short of breath, the body uses up more energy to breathe
- Residents who develop Covid-19 symptoms and become unwell will have specific food and nutrition needs.
Caterers can help by providing:
- Softer/easy chew meals
- Extra sauces to soften food
- Small meals and snacks – for a little and often approach
- Appetising meals served not too cold or too hot
How can care homes support residents at risk of malnutrition?
Catering teams have a role in supporting carers and residents with a food first approach; an effective first line strategy recommended by BAPEN and the BDA.
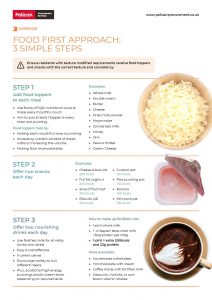
A Food First Approach: 3 simple steps
- Add Food Toppers to each meal
- Offer two snacks each day
- Offer two nourishing drinks each day
Download Practical Guide to Food First Approach: 3 Simple Steps
A caterers’ checklist of practical considerations
- Do the catering team have sight of residents’ nutrition care plans?
- Do the catering team have a list of residents who require a food first approach?
- Does the food trolley include a selection of food items to help with a food first approach for easy access?
- Do the catering team provide a list of snacks, food toppers and nourishing drinks available?
- Are pictures or visual aids available to help residents make food choices?
- Do the catering team have the key ingredients, snacks and drinks in stock?
We are here to help you
If you, or your catering team require help with nutrition for your residents, please contact Pelican’s Dietitian, Anna-Maria Holt RD at anna-maria.holt@pelicanprocurement.co.uk









